Provider payment reform is a transition from traditional fee-for-service payment models to VBP models. Reform is occurring because of a widespread belief that increasing costs under fee-for-service models are not sustainable. VBP models feature payment structures linked to quality and outcomes, which reward both efficiency and effectiveness. The overall goals of VBP programs are to (1) provide better care to individuals, (2) improve the overall health of a population, and (3) reduce healthcare costs. Examples include pay-for-performance programs that reward improvements in quality metrics and bundled payment methods, which pay providers based on an episode of care rather than for individual services provided.
- Value-based payment is designed to give healthcare providers incentives to achieve the Triple Aim:
- Better quality care for patients and satisfaction for patients
- Improved health of the population covered by the payment arrangement
- Lower per-capita cost
- Traditional fee-for-service payments compensate doctors and other health care providers for each service performed with no financial incentive for improving patient outcome.
- Value-based methods, at a minimum, tie payment to quality and/or outcomes of care. "Pay-for-performance" is a type of value-based payment method that maintains fee-for-service payment but adds a financial reward/penalty related to quality/outcomes.
- Other more advanced forms of value-based payment methods provide a financial incentive to provide care more efficiently for an episode of care such as a joint replacement ("bundled payment"), or in "population-based" methods over the course of a year for all services received. In either case, tying payment to quality/outcomes is a key feature.
- Typically providers enter into risk contracts with insurers ina which the annual cost of patient care is tracked against predetermined per-member spending targets. This arrangement creates a financial incentive for the provider to control costs.
- In an "upside-only" or contract, providers are rewarded and share in savings if actual treatment costs are lower than the target, but are not penalized if spending exceeds the target.
- For contracts that also include "downside risk," providers can still earn upside savings, but must pay a share of the added costs if actual costs are higher than the target.
- Contracts with downside risk provide the greatest incentive for providers to manage and lower claim cost.
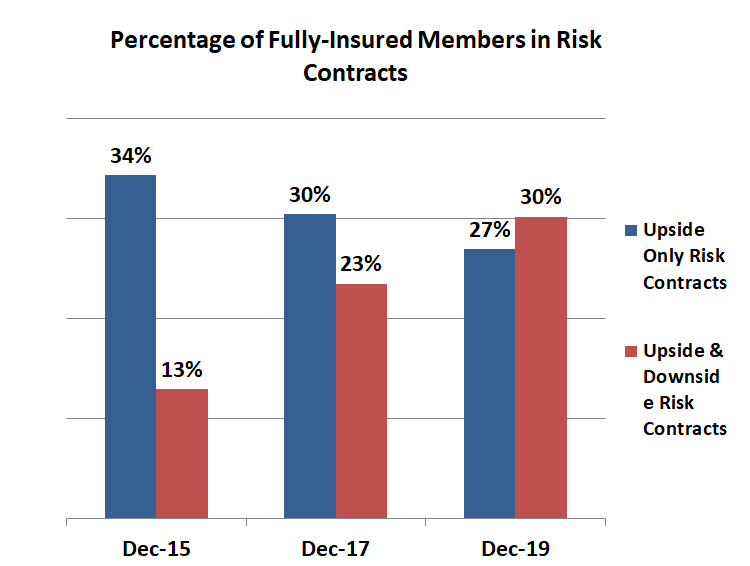
The graph below illustrates growth in the proportion of members in provider risk-based contracts for fully-insured NH plans. In 2015 most risk contracts include provider upside risk only (gain sharing only without downside risk or loss sharing) but that changed over time. 2019 had more providers taking on downside risk than just the upside risk from a few years ago.